Posted on : June 28, 2024

Obesity isn’t just about carrying a few extra pounds. It’s a major global health crisis that’s been snowballing, affecting millions worldwide. But there’s a glimmer of hope on the horizon, and it comes from a perhaps unexpected field: nutritional science. This blog will dive into how the latest developments in this area, often showcased at health conferences like the Health 2.0 Conference, are revolutionizing the way we treat obesity. From genetic-based diets to technological advancements in food tracking, let’s explore these exciting developments and see how they’re changing lives.
-
Understanding Obesity
The Definition And Impact Of Obesity
Obesity is defined medically when a person's body mass index (BMI)—a calculation derived from weight relative to height—exceeds 30. According to the World Health Organization (WHO), global obesity has nearly tripled since 1975. In 2016, more than 1.9 billion adults were overweight, of which over 650 million were obese. Obesity is a leading risk factor for numerous grave health conditions, including diabetes, heart disease, and certain cancers, making its management a crucial public health initiative.
Causes And Contributors
The roots of obesity can be traced to a mix of genetic, lifestyle, and environmental factors that complicate its prevention and treatment. Understanding these multifaceted contributors is essential for developing effective interventions. As we delve into the complexity of obesity, which requires sophisticated approaches where nutritional science plays a crucial role, upcoming 2025 US healthcare events could offer potential opportunities for groundbreaking insights.
-
Role Of Nutritional Science In Obesity
Nutritional science examines how the foods we eat affect our health and well-being. Recently, it has become a cornerstone in understanding and combating obesity, especially with events like those anticipated in the 2025 US healthcare sector. Nutritional scientists are continuously uncovering how different nutrients and dietary patterns affect weight gain and body composition.
For instance, studies have shown that diets high in refined sugars and fats can lead to weight gain, whereas diets rich in fiber and lean proteins may help control it. This evolving field is giving us the tools to fight obesity more effectively than ever before, paving the way for tailored dietary strategies.
-
Nutritional Interventions For Obesity Treatment
Dietary Changes
One of the most effective weapons against obesity might just be your meal plan. Low-calorie diets are a traditional approach, but low-carb and Mediterranean diets have gained popularity for their effectiveness and ease of adherence. Each diet has its merits and can be tailored to individual preferences and medical needs, making dietary strategy a cornerstone of effective obesity management.
Power Of Dietary Fiber
Dietary fiber, often overlooked, plays a vital role too. It helps regulate digestion and can lead to prolonged feelings of fullness, which helps with weight management. Incorporating a high-fiber diet can significantly affect weight control and is a simple, effective strategy anyone can start.
Timing And Frequency Of Meals
Intermittent fasting and mindful meal timing can also play significant roles. These methods aren't just about cutting calories—they're about restructuring our relationship with food. By aligning our eating patterns more closely with our natural circadian rhythms, we can improve our metabolic health and reduce obesity risk.
-
Emerging Trends In Nutritional Treatment Of Obesity
Personalized Nutritional Plans
The field of nutritional science is not just evolving; it's revolutionizing. As seen from discussions at various international healthcare conferences such as the Health 2.0 Conference, personalized nutrition, tailored to individual genetic makeup, is on the rise. This approach allows for diet plans that are uniquely suited to an individual’s genetic disposition, potentially increasing the effectiveness of dietary interventions.
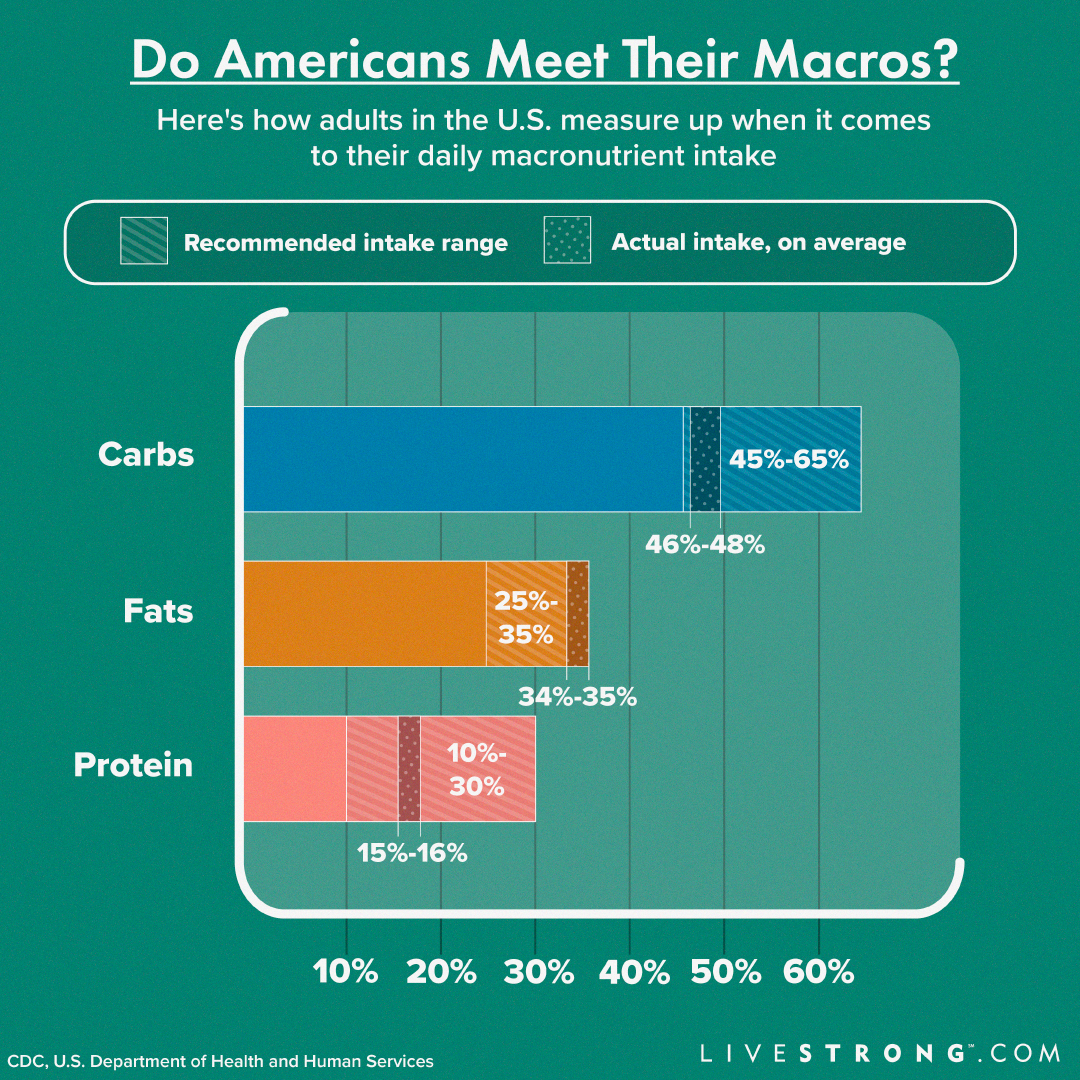
Source:Livestrong.com
Microbiome And Diet
Additionally, understanding the microbiome—the vast community of microbes living in the human gut—has opened new paths for obesity management. This research suggests that altering our gut bacteria through diet can play a crucial role in controlling obesity.
Technological Innovations

Technologies like mobile apps that track food intake and activity are also playing a role, making dietary adjustments more manageable. These innovations are making the treatment of obesity more customized and effective than ever before.
-
Challenges And Considerations
Despite these advances, implementing nutritional changes isn’t always straightforward. Psychological factors, such as stress eating, and social surroundings, can make it hard to stick to dietary plans. Moreover, sustainability is a significant challenge—short-term diets are often ineffective in the long run.
Nutritional advice must also navigate legal and ethical hurdles, especially when it comes to privacy and personal data use in genetics-based diets. These challenges highlight the need for comprehensive strategies that consider all aspects of an individual’s lifestyle.
-
Future Directions
Nutritional science is poised at the edge of new frontiers in obesity treatment. As research delves deeper, we can expect more breakthroughs that will continue to shape how we understand and manage obesity. Collaboration is key—healthcare professionals, including dietitians and nutritionists, must work together to integrate these advances into effective treatment plans. Moreover, public health policies could significantly influence these treatments by promoting healthier environments and food choices.
-
Conclusion
As we've seen, nutritional science is not just about understanding what we eat but about unlocking the potential of diet to combat obesity. While the challenges are significant, the continuous advancements in research, such as those presented at health conferences like the Health 2.0 Conference, provide hope and practical paths forward. By staying informed and proactive, we can all contribute to a healthier future.
FAQs
- What recent advances in nutritional science are most promising for obesity treatment?
Recent advances include the development of genetic-based diet plans and technological tools like food tracking apps. These innovations allow for more personalized dietary strategies, improving the effectiveness of interventions tailored to an individual’s specific health needs and genetic predispositions.
- How does nutritional science contribute to obesity management?
Nutritional science dissects the relationship between diet and health, offering crucial insights into obesity management. It helps develop dietary strategies tailored to individual health needs and preferences, such as low-carb or Mediterranean diets, which have been effective in managing and reducing obesity.
- How does the Health 2.0 Conference address the intersection of education and nutritional science in combating obesity?
The Health 2.0 Conference integrates discussions on how educational frameworks can incorporate nutritional science to combat obesity. It emphasizes creating curricula that include comprehensive nutrition education, encouraging students to develop healthy eating habits and understand the implications of diet on overall health.
- What challenges does nutritional science face in the treatment of obesity?
One of the main challenges is the implementation of effective, long-term dietary changes. Factors such as psychological eating behaviors and social environments often complicate adherence to nutritional advice. Additionally, legal and ethical considerations, particularly in genetic-based nutrition plans, pose significant hurdles.
- What educational strategies are being discussed at the Health 2.0 Conference to promote better nutritional understanding among students?
The Health 2.0 Conference explores strategies like incorporating nutrition topics into the standard curriculum, developing school-based health initiatives, and utilizing digital tools to teach students about balanced diets. These methods aim to empower students with the knowledge necessary to make informed dietary choices and actively manage their health, building a foundation for lifelong healthy habits.











